The VasClip® Procedure
an assessment by Dr. Doug Stein after performing four VasClip procedures
Note: Most of this page was written a few days after performing four VasClip procedures in one day (7/23/04). At the time of the follow-up semen checks months later, we learned that of the four patients on whom I performed the procedure, two experienced early failure, persistence of live sperm in the semen beyond 12 weeks after the vasectomy. This 50% early failure rate was not acceptable and I stopped performing the VasClip procedure. Supporting my personal findings is an article published in the Journal of Urology, Volume 176, page 2146, November 2006: Levine et al at Rush University Medical Center in Chicago performed 8 VasClip procedures, of which 2 failed, for a 25% failure rate. But you may read on if you are curious about the principles involved.The VasClip



The vas tubes can be blocked by simply pinching a spot closed, as one would stop the water flow in a thin-walled garden hose by stepping on it or compressing it with enough force to collapse the inner walls. This could be accomplished by tying the vas with a suture or by applying a metal hemoclip, a V-shaped piece of titanium (half the size of a paper staple) that is compressed closed with a hemoclip applier. The problem with sutures and hemoclips is determining how tight to make them: too loose and the vas tube may not be crimped completely closed, allowing sperm flow to continue ... too tight and the underlying tiny portion of the vas tube (which is living tissue) could simply waste away from lack of blood supply, allowing the ends on either side to establish channels around the compressed site through which sperm could flow once again, resulting in failure of the attempt to permanently stop the flow. I suspect that a universal happy medium does not exist because of the variations from man to man in vas size and resilience.
The VasClip was an ingenious device (about the size of a hemoclip) that was designed to compress the vas tube tightly enough to close the vas and stop the flow of sperm, but not so tightly that the blood supply to the underlying portion of vas is damaged. Since the underlying vas supposedly remains healthy, there is no tissue injury, and collateral channels should not form. Before reading about my impressions of the VasClip procedure, I would have you view the VasClip website, but the site is no longer online, as VasClip has been taken off the market. While I have no personal experience with the Pro-Vas device, and since there may be significant differences between it and the VasClip which will make it more effective, the the Pro-Vas website seems to indicate that it also works by simply crimping the vas.
When any clip-like device is used, the surgeon does not change his method of applying local anesthesia (either a needle or a spray applicator), nor does the surgeon change his method of accessing the vas tubes (either the traditional method of making one or two small incisions or the no-scalpel technique). All that changes is the third phase of the procedure (the method of stopping the flow of sperm), which is the phase which involves no discomfort, so use of the VasClip or Pro-Vas does not influence the chances of having discomfort during the vasectomy. Some patients feel some discomfort during application of the anesthetic, and a few patients feel discomfort during the process of accessing the vas, depending on the thoroughness of the surgeon in applying the local anesthetic. But once a small section of the vas has been lifted through the opening in the scrotal skin, nearly all patients feel nothing because there are no nerves right on the surface of the vas.
There are two potential benefits of the VasClip or Pro-Vas:
(1) During either procedure, none of the vas is injured because no section of the vas is removed or cauterized or "tied off". Whether this, and the fact that there is no sperm leakage at the vasectomy site, mean that patients will have less post-procedure discomfort remains to be seen. (Here I am using the word "vasectomy" to refer to any procedure performed on the vas tubes for purposes of achieving sterility. Technically, the VasClip procedure is not a "vasectomy" in the strict sense of the word because no portion of the vas is cut, removed, or cauterized.) We need questionnaire-based studies that compare post-vasectomy discomfort with post-VasClip discomfort in patients who undergo vasectomy and VasClip procedures by the same surgeon. Since most of my no-scalpel vasectomy patients have negligible post-vasectomy discomfort and many have no post-vasectomy discomfort, we would need to obtain questionnaire-based data from a large group of patients (perhaps hundreds) to achieve statistical significance and make the study valid. My impression after four VasClip procedures is that the VasClip does not decrease discomfort to a level even lower than what it is with NNNSV (no-needle no-scalpel vasectomy).
(2) Although no adequate VasClip reversal data is available, reopening the obstructed portion of the vas might be possible by simply removing the VasClip. This would certainly make the reversal process very quick and simple. I have performed reversals on two men in whom VasClips were used, and this was not the case. The VasClips were encased in thin capsules if scar tissue that made them difficult to remove, and I had to divide the vas tube and perform traditional reversal connections. But even if simple removal were possible, the VasClip procedure cannot be considered "reversible" because the inflammatory process required to absorb and recycle sperm after the procedure can damage the tubes (especially the epididymis) upstream from the VasClip site resulting in scarring and sites of secondary obstruction. However, there is little doubt in my mind that reversal of VasClip procedures is technically easier than reversal of a traditional or no-scalpel vasectomy for two reasons: (1) since the vas is not divided, there is no gap between severed ends created by removal of a section of vas or retraction of the ends (accessing widely separated vas ends can be a challenge during vasectomy reversal), and (2) since the vas is not divided, there is no leakage of sperm at the VasClip site and there is likely to be less inflammatory scar tissue at a VasClip site than at a vasectomy site.
There are four potential drawbacks to use of the VasClip or any crimping device:
(1) High early failure rate and unknown late failure rate.
While the VasClip website provided data which collectively presents a failure rate for traditional vasectomy of 4.1%, I think that the failure rates of traditional and no-scalpel vasectomy are much lower than this in the practices of experienced vasectomists. Since initiating the techniques that I presently use in August 1990 (with a minor modification in February 2007), only 12 of over 25,000 men (about 1 in 2000) have experienced "early failure" (prolonged persistence of motile or numerous sperm in the semen after vasectomy), presumably due to early reattachment of the vas ends or growth of collateral channels, and only seven of over 25,000 men (about 1 in 3000) have experienced reappearance of sperm in the semen resulting in pregnancy ("late failure") after they were told that their semen was free of sperm, presumably due to late development of collateral channels. This is a failure rate of less than 0.1%.
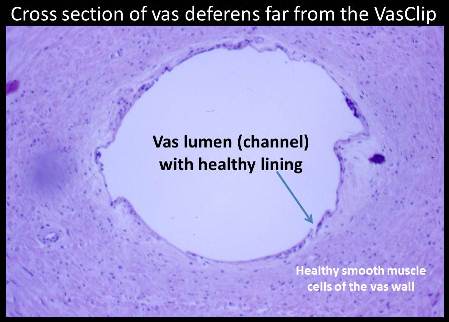
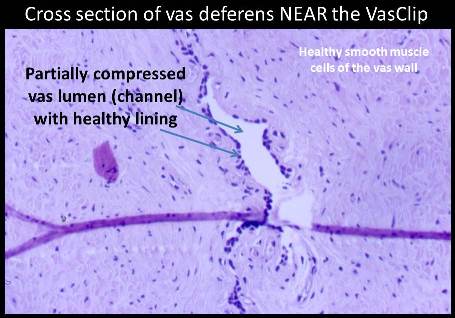
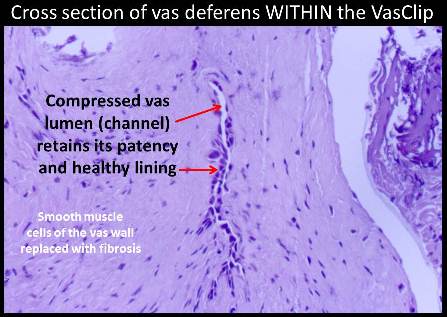
Of the four patients on whom I performed the VasClip procedure in the presence of the founder of the company, two experienced early failure. This 50% early failure rate is not acceptable and I no longer perform the VasClip procedure. The other two patients became sperm-free, but they are aware of the other two early failures and they have been encouraged to have their semen checked periodically for the delayed reappearance of sperm (late failure). The photos below were taken during the repeat vasectomy (on 2/23/05) of a man who had experienced VasClip failure.
Section of the vas with VasClip intact lifted through a small scrotal opening. The section was removed ...
...and one can barely see the opening of the cut vas. Water passed through the vas even before the VasClip was removed, confirming the patency (openness) of the vas.
(3) While there is variability of vas tube thickness from one man to another, there is only one VasClip size. The VasClip cannot be used in men who have very thick vas tubes. This is not a significant problem for men who have separate consultation and procedure visits, because the thickness of the vas tubes will be evident on physical examination at the time of the consultation visit, and the VasClip candidate can be either reassured or told that his vas tubes may be too thick for the VasClip when he returns for his procedure. However, some men, especially those who travel a long distance to a particular surgeon, may prefer to have their consultation and procedure visits on the same day. After psychological preparation for the VasClip, after time spent on the phone trying to convince his insurance company to cover the cost, and after a long drive to the office of a VasClip surgeon, the anxious candidate may be very disappointed to learn that his procedure of choice was not possible.
(4) Cost. To a surgeon, the cost of each one-time-use VasClip kit was $300 - $400, depending on the number of kits ordered. This increased cost must be passed on to the patient. Since anesthesia and exposure of the vas tubes is the same for traditional/no-scalpel and VasClip procedures, use of the VasClip can save time only during the third phase of the procedure (creating the blockage either by dividing the vas and managing the ends or by applying a VasClip). I could see after only a few VasClip procedures that the VasClip would save some time compared with my usual technique, but the time savings was less than 30 seconds (less than 5% of the total procedure time) and not enough to justify reducing the fee. When the VasClip was available, a few insurance companies who covered vasectomy under certain plans were offering a higher rate of reimbursement for the VasClip procedure. This may also be the case with the Pro-Vas device.Other surgeons may have a very different view of the VasClip and ProVas procedures. Some may see great merit and some may focus on the potential drawbacks.
My overall impression of vas crimping devices is not favorable, because of the high failure rate in my practice of the VasClip. The Pro-Vas device may have subtle design differences that reduce the failure rate and I look forward to reading reviews about its effectiveness.
Return to the vasweb Vasectomy Page